Welcome to Start TODAY. Sign up for our Start TODAY newsletter to receive daily inspiration sent to your inbox — and join us on Instagram!
One day in March 2023, Kyle McMorrow of Brooklyn woke up at 5 a.m. with the worst neck pain he’s ever had. “I thought I had slept on it wrong. I tried to massage it out with a massage gun, but nothing worked,” he tells TODAY.com.
He was 36 years old, healthy and active — he worked out in a gym, played basketball, biked outdoors, ran and hiked. It never crossed his mind that he could be having a stroke.
Despite the pain, he headed to his job in New York City, but he noticed some unusual symptoms. “As I took the train to work, I was having a hard time walking in a straight line. It felt like there was a magnet on my hip pulling me to the left. I didn’t understand what was happening,” he says. He also started feeling nauseous.
When McMorrow arrived at work, he talked to his boss about his symptoms, and his boss told him he should see a doctor.
McMorrow decided to see his primary care doctor. While he was waiting for the train, he called his girlfriend, Ema Jimenez, who knew something was seriously wrong.
“His speech was slurred. When I heard that, I thought it might be a stroke, but I didn’t tell him that,” she says. “It seemed neurological to me. I had meningitis once, so I know what it feels like when your symptoms don’t really let up and you feel nauseous like that,” she says.
She told him he needed to go to the hospital, and he took her advice. McMorrow says, “When I got out of the train station, I still didn’t understand what was happening. I was looking for a cab. I stumbled around for about ten minutes. If you saw me in the street, you’d probably think I was drunk or on something because I was crashing into light poles, crashing into parked cars, and stumbling block by block. I couldn’t understand what was wrong. I probably should have called 911, but I finally got a cab.”
The cab took him to the emergency room at NewYork-Presbyterian/Lower Manhattan Hospital, where the staff knew right away that something serious was going on.
Testing and specialists confirmed what Jimenez had suspected: McMorrow was having a stroke. The team transferred him to NewYork-Presbyterian/Weill Cornell Medical Center for the treatment he needed.
Jimenez recalls meeting McMorrow at the hospital: “The left side of his face was droopy, and his vision had started to blur. He was shaking. He was just not in good shape.”
McMorrow has some memories of his symptoms: “There’s a lot I don’t remember, but I remember being very aware of the things that I didn’t have anymore. The ability to feel throughout my body was gone, and so was my vision, my speech, my swallowing and my standing. Those things, I was very aware of.”
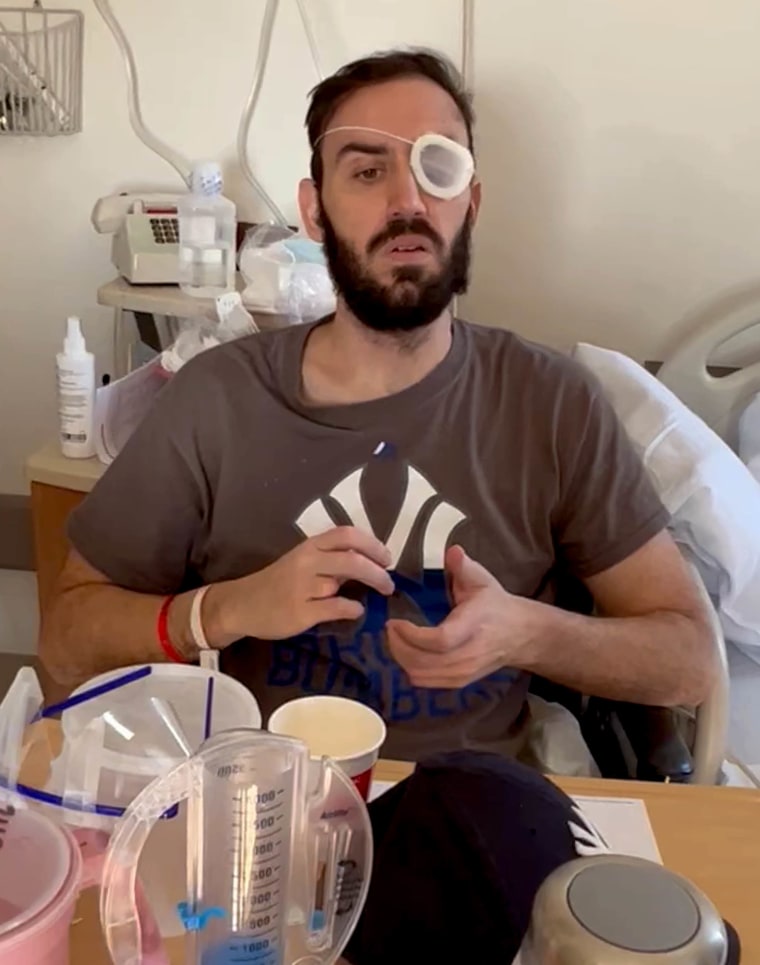
Bleeding near the brainstem was causing scary symptoms
McMorrow was diagnosed with a cavernous malformation, a rare condition that causes a cluster of abnormal blood vessels. Sometimes, these vessels are stable, and people don’t even know they have the condition. But other times, the blood vessels can leak, and the bleeding can cause serious symptoms.
In McMorrow’s case, the malformation was on his brain stem, and it had burst. The area filled up with blood and caused the stroke. “I found out later on not everyone survives,” he says.
Sometimes, surgery can treat cavernous malformations. But experts thought it would be too risky for McMorrow — it might leave him paralyzed.
McMorrow was afraid he would never be able to have surgery. “They were nervous to go in unless it was life or death because it was on the brainstem,” he says. “I did not want to worry every time I had neck pain that it was happening again. In my mind, that’s no way to live — always guessing. Always being nervous.”
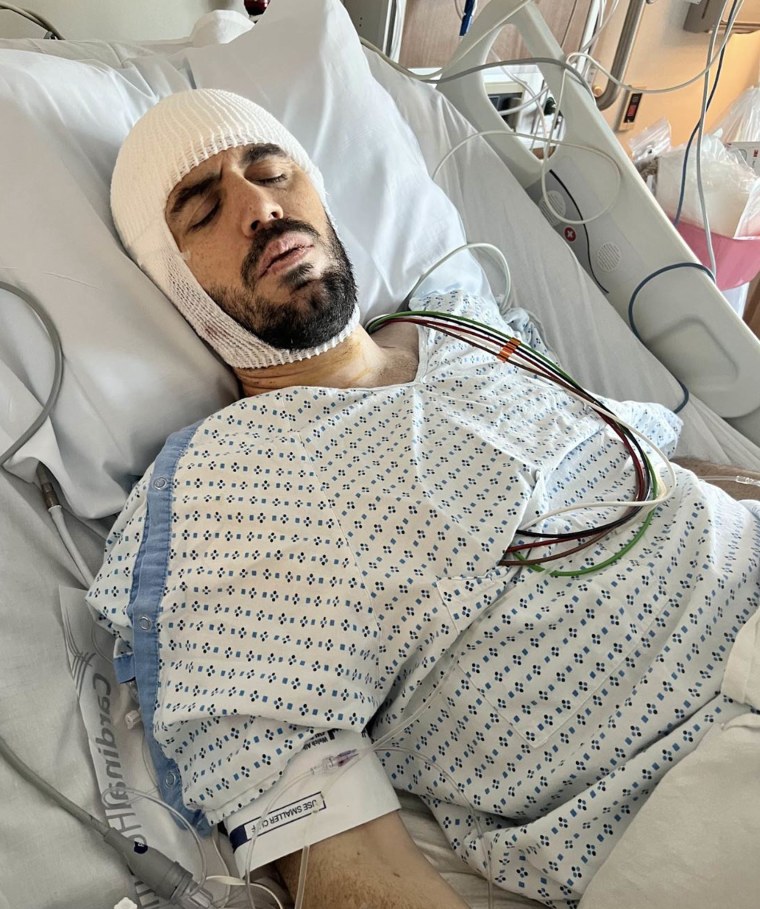
The healthcare team gave him steroids to help his body reabsorb the blood. He was in the intensive care unit for ten days, in a regular hospital room for two days, and then moved to in-hospital rehabilitation for about four weeks. Over that time, MRI scans monitored the amount of blood in the area of the malformation.
At first, McMorrow couldn’t even stand. It was difficult for him to do anything. He had to relearn how to walk, go up stairs and get in and out of the shower. His swallowing was so weak that he needed a liquid diet, and his speech was slurred.
“When I could see that he couldn’t walk, and he could barely even sit up, I was thinking, ‘OK, if this is how things are going to be, I need to prepare myself. How do I take care of him?’” Jimenez says.
Thanks to a team of physical, occupational and speech therapists working with him six days a week, three hours a day, McMorrow regained his strength and skills. He learned to balance and walk. His speech became clear again and he could eat solid food. His vision improved, though he still wears prism glasses to help with double vision in his left eye.

A treatment opportunity opens up
About six weeks after McMorrow’s stroke, scans showed that the malformation had shifted, a lot of the blood had been reabsorbed and it would be safer to operate. “I called so many people to tell them it was the greatest news I could hear. Brain surgery sounds very scary, but the other option was to live like this for the rest of my life. I didn’t want that,” he says.
His surgery, which took seven hours, was on May 30, 2023. For eight weeks afterward, he couldn’t do anything strenuous. “Since then, I’ve slowly gotten better. I’ve had follow-up MRIs, and they seem clean. By all accounts, it was a success,” he says.
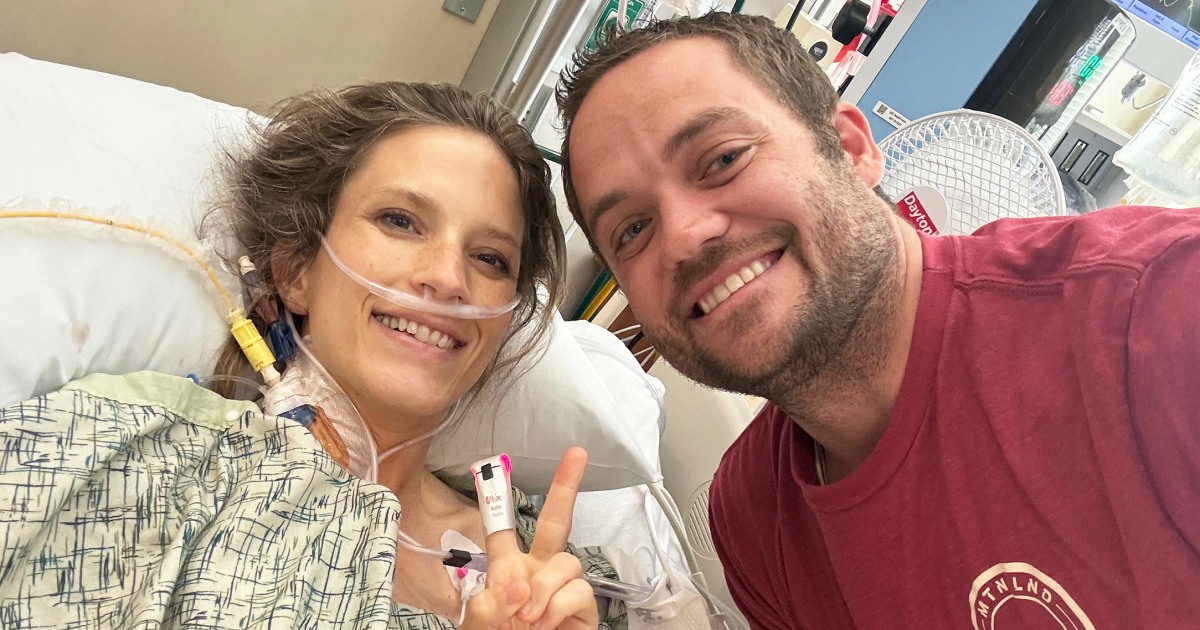
Getting home felt like a milestone. “All I wanted was to return to my normal life. I felt like it had been taken from me. When Ema got me home, it was the greatest feeling,” he says. “It wasn’t just being home and being in my own space, but feeling comfortable in my own body again. They went hand in hand.”
He appreciates the fitness level he had before his stroke, and he thinks it helped with his recovery: “Being somewhat in shape coming into the incident, and being very physically active, I think it went a long way. I feel very blessed and lucky to be where I am today. I lost most of my motor skills and everything that goes with that in March, and by the middle of July, after that eight-week period after the surgery, I was back at work. It’s incredible to think back about where I was to where I am,” he says.
Read the full article here